 Written by Sara McEvoy, PT, DPT
Written by Sara McEvoy, PT, DPT
Sports medicine is a highly rewarding and in-demand field of rehabilitation that helps people recover from sports-related injuries, avoid recurring dysfunction, and maximize physical performance.
Healthcare providers who are most often involved in sports medicine care include orthopedic surgeons, physicians, athletic trainers, physical therapists, occupational therapists, kinesiologists, and exercise physiologists.
These sports medicine practitioners may be involved at virtually any point of an individual patient's athletic career. For instance, exercise physiologists and physicians may be involved in screening and preventive programs (in addition to diagnosis and treatment). Athletic trainers often provide on-field assistance within moments of an initial injury. Physical therapists and occupational therapists are often involved in diagnostic and therapeutic stages within the acute, subacute, and/or pre- and post-operative windows.
Interdisciplinary collaborative communication is essential for appropriate continuity of care and optimal patient outcomes, whether the patient is an elite level competitor or a novice athlete with multiple comorbidities.
Additionally, at no point during a patient's journey with sports medicine should he or she take a passive role in their care. Full engagement, including advocacy (for themselves or for dependents under their care) and participation in active and manual therapies, is a must for timely return-to-play, return-to-work, or any other objective and subjective measures of improvement.
Patients should also be educated about their injury or condition and empowered to understand how participation in their recovery will help them regain or even surpass their prior level of function and performance.
What's one way to increase patient motivation and engagement? Keep their sports medicine rehabilitation challenging, interesting, and relevant to their goals.
No sports medicine program would be complete without a diverse range of equipment, devices, and services that can be used to help athletes of all ages and abilities recover from injury and meet the specific objectives of their rehab. Such objectives may include:
Naturally, these objectives are variable from patient to patient and will depend on factors including individual goals, needs, injury type and severity, and stages of recovery. And while sports medicine equipment should be selected and utilized based on the typical patient population of a particular practice setting, a lot of the equipment used in this field is highly versatile and can be applied to a wide variety of patients.
The following examples of sports medicine equipment can be used to implement treatment, modify and progress treatment plans, and provide objective measures that are important for the evidence-based, outcomes-based model of modern-day rehabilitation. These services and devices can also help a patient stay safe and motivated throughout their plan of care.
Functional exercise equipment encompasses a versatile and diverse range of tools and devices that permit patients to perform multi-joint, compound movements that resemble or directly mimic real-life tasks, including sports-specific skills.
Functional exercise equipment may include:
These tools give a patient the opportunity for safe strengthening, proprioceptive awareness, and skill development by allowing them to practice task-specific elements of their sport or craft before integrating them back into a full training or competitive movements.
Functional exercise equipment (and the movements performed with them) can also be easily modified to reduce the possibility of activating uninjured or uninvolved muscles, based on the clinical judgment of the treating practitioner.
Safety of the patient is always the number one priority, and functional exercise equipment should always be selected with this in mind. It's important to consider the patient's injury stage, injury severity, and past medical history, as this can influence which pieces of equipment will be the most appropriate for them.
Many of the above equipment can be combined to enhance safety or make a therapeutic task harder or easier (for instance, placing a wobble board inside a set of parallel bars to provide incidental upper extremity support and promote reactive balance strategies).
Braces and supports, including orthoses, shoe inserts, and splints, have several potential indications. They can be used to:
However, special considerations should be taken when deciding to fit for and prescribe these types of supportive equipment. For instance, back braces and similar devices often provide patients a false sense of security during their sports- or exercise-related activities. It is up to the clinician and the patient to ensure that the patient is able to demonstrate the requisite strength, endurance, form, and body awareness to perform a movement safely even if a brace is worn, with or without load.
Special considerations also need to be made when selecting braces and supports for patients with additional comorbid conditions, such as impaired sensation or poor skin integrity. Brace material, as well as the ease with which a patient can don or doff the brace (or direct others to do so), must be taken into account in order to minimize the risk of complications.
 | AnkleSTONE Foot and Ankle Stretcher | Made in the USA! View Product |
So many grand promises and stars have lost their career due to a badly handled injuries. Getting injured is part of the job for all athletes, so the crucial part resides in how injuries are treated. Ankle injuries are maybe the most common type of all no matter what sport you are in. Tennis, Golf, Trail Running, Football, Basketball, Hockey, and Baseball are full of great players struggling to recover from an ankle injury since they're as frequent as sensitive. The good news is that the AnkleStone Foot and Ankle Stretcher provides a solution to most foot and ankle injuries that can be accessed anywhere at any time. Its design is portable, lightweight, and painless.
Starting the path to a whole recovery is easier when the AnkleStone is treating you. Simply place it on the ground and step gently into it to let its curve-shaped surface accommodate muscles and increase your range of movement. This treatment uses safe, painless, and natural body movements to help you recover and go back faster to your prime level.
To support athletes on the go, the AnkleStone was created with a convenient size that will fit any sports bag and is also lightweight. Athletes can get quick relief before, during, or after every game. Especially useful for weekend sports events. The AnkleStone boosts strength in foot and ankle muscles while increasing flexibility through natural and painless movements. Therapists and athletes suggest this as one of the best ankle injury rehabilitation processes.
As mentioned, the more actively involved a patient is in their rehabilitation (e.g., learning and performing exercises and stretches), the better their outcomes will be. However, manual therapy and other types of more "passive" treatments still play important complementary roles in many plans of care.
Devices can be used in sports medicine that can assist the practitioner as he or she provides manual therapy techniques, including spinal traction devices. These tools can be instrumental in practice settings with a high degree of athletic patients and heavy caseload, because it can reduce the risk of job-related strain on the clinician and improve the overall effectiveness of the manual intervention.
Additionally, many manual therapy tools such as foam rollers and massagers, allow the patient to perform self-mobilization and manual therapy techniques as part of a home exercise program. This can enhance and accelerate the overall effectiveness of a patient's entire plan of care.
Functional exercise equipment can certainly be used to enhance strength and provide safe, graded resistance to therapeutic exercises. But resistance training in the sports medicine setting can also be enhanced with pulleys, resistance bands, and similar tools. Pulleys and resistance bands can be particularly effective at performing single joint movements and helping patients avoid compensatory action, as in the example of rotator cuff stabilization exercises.
Many of these tools, including resistance bands and tubing, can be provided to patients as part of their home exercise programs for continued training outside of clinic appointments.
For athletes who need to improve motor control, body awareness, and muscle-specific strength and activation, adding modalities such as biofeedback to resistance exercises can enhance overall training affects.
Pain is valuable feedback to an injured athlete. But managing this pain appropriately is essential for any patient undergoing sports medicine treatment. Not only does pain impair a person's quality of life and increase psychological stress, but it can also disrupt a person's ability to actively and effectively participate in their rehabilitation and therapeutic exercises.
Providing hygienic, cost-effective, and effective hot and cold therapy modalities including cold packs, heat packs, and even therapeutic ultrasound and diathermy can produce various degrees of tissue heating at various depths to reduce pain, promote increased circulation and cellular metabolism, and reduce or control swelling, and inflammation.
Sometimes, no amount of active exercise or manual therapy will be enough to adequately reduce or eliminate swelling and fluid retention in an injured area, especially if additional systems including lymphatic drainage are involved in an injury.
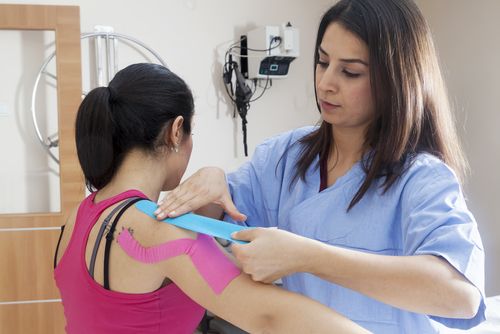
In these cases, the use of compression garments, bandages, kinesiotape (athletic tape), and related tools may be instrumental in progressing the patient's injury and managing his or her symptoms. In other cases, active and manual therapy is effective but further enhanced through the use of these tools.
Athletes with postural imbalances or body awareness issues can also benefit from kinesiotape since it provides tactile feedback, especially when applied to the patient's skin while he or she is positioned in an "optimal" posture. Because kinesiotape also improves local circulation, it can also assist with pain relief, swelling reduction, and range of motion.

Sports medicine practitioners work with athletes of all ages, abilities, and backgrounds. Many patients come into sports medicine care because of acute or chronic injuries that are impairing their ability to participate in the sport or activity they love, or even engage in meaningful and productive work and leisure activity. Common injuries include:
A sports injury can occur in any level of athletic endeavor and may affect any level of athlete, including competitive team players and solo "weekend warriors." Any and all of these patients suffering from sports- or exercise-related injury can benefit from individually tailored sports medicine care, part of which must involve identifying and addressing underlying risk factors.
These risk factors may include:
Unlike an annual exam which includes a more generalized assessment of a patient's physical health, a sports physical is helpful for determining if an athlete is in good enough physical health safely participate in the demands of sport or exercise. These are particularly useful for athletes because it can help them learn about specific areas of imbalances, weaknesses, or other underlying factors which could be increasing their risk of injury.
According to the American College of Sports Medicine, the goals of a typical pre-participation sports physical are to:
In some cases, sports physicals are required for legal and/or insurance reasons, especially among school-aged student athletes.
As mentioned, healthcare providers who are commonly involved in sports medicine treatment and prevention include physicians, orthopedic surgeons, exercise physiologists, kinesiologists, physical therapists, occupational therapists, and athletic trainers.
Additional providers may include acupuncturists, massage therapists, sports psychologists, personal trainers, podiatrists, and sports nutritionists or dietitians.

Most of the equipment that can be found in a sports medicine-related facility is highly versatile and can be safely used with and accommodated for a variety of patients.
However, each practitioner and clinic should consider the needs of their patients on a general level, as well as the specific characteristics of individual patients when selecting the equipment that will be both most beneficial and maximally cost-effective.
To see more of the equipment that can enhance your sports medicine practice, browse our full selection at RehabMart today.
If you liked this article and want to learn more about our clinical recommendations, featured products, and the best caregiver tips and tricks, be sure to visit Caregiver University.

Sara McEvoy, PT, DPT, is a licensed and board-certified Doctor of Physical Therapy. She has direct clinical experience within the long-term acute care and skilled nursing settings, and has a special interest in geriatrics and neurological rehab. She is also a freelance writer who creates content almost exclusively within the health and wellness fields.